Article Text
Abstract
Recent military conflicts in Iraq and Afghanistan have resulted in the significant increase in blast-related traumatic brain injury (TBI), leading to increased Department of Defense interest in its potential long-term effects ranging from the mildest head injuries termed subconcussive trauma to the most debilitating termed chronic traumatic encephalopathy (CTE). Most patients with mild TBI will recover quickly while others report persistent symptoms called postconcussive syndrome. Repeated concussive and subconcussive head injuries result in neurodegenerative conditions that may hinder the injured for years. Fundamental questions about the nature of these injuries and recovery remain unanswered. Clinically, patients with CTE present with either affective changes or cognitive impairment. Genetically, there have been no clear risk factors identified. The discovery that microglia of the cerebral cortex discharged small extracellular vesicles in the injured and adjacent regions to a TBI may soon shed light on the immediate impact injury mechanisms. The combination of neuroimaging and advanced research techniques may, one day, fill critical knowledge gaps and lead to significant TBI research and treatment advancements.
- brain injuries
- traumatic
- brain concussion
- Glasgow Coma Scale
- war-related injuries
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
Highlights
Each year, 1 700 000 people in the USA sustain traumatic brain injuries (TBI) from which 52 000 will die. TBI is the contributing factor to 30% of all injury-related deaths in the USA and there are 3.2–5.3 million people in the USA currently living with TBI-related long-term disabilities.
Recent military conflicts in Iraq and Afghanistan have resulted in the significant increase in blast-related TBI.
Possible links between TBI, post-traumatic stress disorders and suicide are suspected and perhaps even probable.
Most patients with mild TBI will recover quickly while others report persistent symptoms called postconcussive syndrome.
Repeated concussive and subconcussive head injuries result in neurodegenerative conditions that may hinder the injured for years if not in perpetuity.
Genetically, there have been no genes described as clear risk factors, although apolipoprotein E4 carriers have been reported to suffer more severely after TBI.
Microglia of the cerebral cortex discharge small extracellular vesicles in the injured and adjacent regions to a TBI which may soon shed light on the immediate impact injury and secondary injury mechanisms.
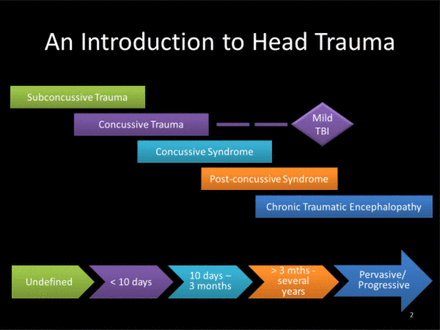
The current understanding of head trauma views concussion and traumatic brain injury (TBI) as injuries that exist along a spectrum, rather than as discrete events. The mildest head injuries are termed subconcussive trauma and the most chronic, debilitating events lead to profound systemic dysregulation known as chronic traumatic encephalopathy (CTE).1 Subconcussive events are believed to be those injuries that incur brain damage but do not result in noticeable symptoms.2 3 More severe than subconcussive events are minor TBIs where the head either strikes, or is struck by, an object.2 During impact to the head, the brain is pushed against the inside of the skull which can cause bruising, bleeding, and tearing of nerve fibers. Although widely varied, symptoms of a concussion can include headache, dizziness, slurred speech and fatigue among many others.4 Usually, given time and adequate rest, or cessation of at-risk activity, the symptoms of a concussion resolve within 10 days. However, if these symptoms persist, the classification of the injury changes and is dependent on the length of time before symptom resolution. If symptoms linger for longer than 10 days but less than approximately 3 months, the concussion has become a concussive syndrome.5 6 If symptoms persist for longer than 3 months, up to and including several years, the injury is no longer seen as a single episodic event and is termed postconcussive syndrome.6 7 If the symptoms become pervasive and/or permanent, this chronic outgrowth of head trauma is known as CTE.7 Currently, the only definitive diagnosis for CTE is a postmortem examination of brain tissue.1 Most tragically, the clinical features of CTE often mirror characteristic of Parkinson’s disease and Alzheimer’s disease, and like these two devastating conditions there is no known cure for the malady of CTE.8–11 A graphical depiction of the spectrum of head trauma can be found in figure 1 and table 1.
The spectrum of traumatic brain injury (TBI).
Syndrome clinical manifestations
The constellation of symptoms after a concussion or head trauma is both complex and problematic. Proper diagnosis, treatment, and prediction of outcomes after any gradation of head injury are difficult and prone to significant error and subjective bias.1 Due to the heterogeneity of symptom presentation and the disparate factors underlying pathology, in addition to probable genetic precursors (eg, apolipoprotein E12–14 and allelic inheritance), accurate assessment of injury, severity, and recovery is nearly impossible at this juncture.11
Despite the greater awareness and pronounced increase in funding of research into TBIs, TBI still imposes a significant societal burden in terms of lost work time,15 16 medical care costs,17 18 and neuropsychiatric complications.19 20 Each year in the USA, at least 1 692 000 people sustain TBI. This includes 52 000 deaths, 275 000 hospitalizations, and 1 365 000 patients treated and released from an emergency department.21 TBI is a contributing factor to 30% of all injury-related deaths in the USA. It is estimated that 3 200 000–5 300 000 persons currently live with long-term physical and neuropsychiatric disabilities attributable to TBI.22 Even with the increased focus on the assessment of TBI of all severities, much work remains to be done to fully elucidate the various causes and outcomes along the spectrum of injuries. After the publication of the preceding work, significant cross-modal, multicenter studies in TBI risk factors, etiology, assessment and outcomes have been undertaken, with varying degrees of success.23 Researchers are increasingly skeptical of the discovery of the ‘magic bullet’, one-size-fits-all biomarker of neuronal or systemic damage as a clear, indisputable indicator of TBI. Current studies are shifting the onus towards the formulation of the aforementioned ‘trauma panel’: a compendium of proteins or biomarkers whose dysregulation and presence in cerebral spinal fluid or the peripheral blood may be indicative of a level of central nervous system disruption, neuronal damage or systemic loss of homeostatic balance. Recently, the Food and Drug Administration approved a ‘concussion test’ via peripheral blood draw that assesses the presence/level of a pair of proteins in the peripheral blood: glial fibrillar acidic protein and ubiquitin carboxy-terminal hydrolase L1 at 12 hours after a suspected injury.24–27 This is exciting news because we specifically highlighted these proteins, among others, earlier in our work.28 However, this is only one of many steps that need to be undertaken to paint a fuller picture of this troubling disease/condition.
These new discoveries and the renewed focus on the course and impact of TBI have laid the groundwork for some truly novel experimental approaches and collaborative efforts. Perhaps some of the most fertile and untapped territory, however, is the design and implementation of head injury studies focusing on armed services personnel currently deployed, or returning from deployment, in the Middle East and other combat zones. Significant numbers of men and women in uniform sustain TBI resulting from, and in conjunction with, injuries sustained in combat. In contrast to even some of the most rigorously designed multicenter studies of head trauma in academic centers, inclusion criteria for a TBI study involving armed services personnel would be relatively straightforward. Postacute and rehabilitation care provided to uniformed service members by the military could be more centralized which would significantly aid in data collection and patient stratification. The significance of focusing on those returning from combat deployment is readily apparent: they suffer the worst injuries/TBIs (with the possible exception of athletes in contact and combat sports), have the most difficult to diagnose and triage combination of symptoms, and exhibit the poorest outcomes.29 30 Additionally, links and potential cross-pollination with post-traumatic stress disorder (PTSD)31 32 and the societal impact have been acknowledged and require further study. Well-designed and implemented studies with proper triage, outcome assessments and multidisciplinary approaches will elucidate previously unknown linkages between TBI and various ailments (PTSD, neuropsychiatric dysregulation, and so on) and facilitate applicable conclusions and treatments to the general populace and/or other at-risk groups (contact and combat sports participants).
We are on the cusp of a new age in TBI research and treatment and we believe that a proteomic and genomic approach to the study of this disease is vital to the discovery of its cure and treatment. Overall, there is a paucity of serum diagnostic, predictive and prognostic biomarkers in TBI and CTE to help in the early identification, predictions for response to treatment, and aid in treatment selection. There is thus an urgent need to identify novel blood-based biomarkers, that is, liquid biopsy for TBI and CTE. Liquid biopsies offer a rapid and minimally invasive technique to detect and evaluate these injuries and their progression. By analyzing those biomolecules (miRNA, mRNA, mDNA and proteins) that circulate in the potentially injured individual’s serum/plasma and other body fluids, a liquid biopsy can be developed to easily and quickly diagnose if a service member on a battlefield or athlete in their arena has suffered a potential life-challenging injury, allowing leaders to know whether they can be put back into the arena or removed from this theater.
Recent investigations have shown that exosomes, membrane-bound nanovesicles (30–150 nm) released from cells, play an important role in physiologic processes and intercellular communication.33 34 The role of exosomes in brain disease including TBI is still in its infancy but may hold promise as biomarkers as well as drug targets. Exosomes are excellent targets for liquid biopsy as they are easily detected in the serum and are stable at room temperature for hours.35–38 Recent studies in cancer have suggested that specific exosomal miRNAs can serve as biomarkers and have also only begun to be investigated for their diagnostic, prognostic and theranostic properties.
Recently, using diffusion tensor imaging (DTI), blast-related TBI was shown to involve traumatic axonal injury.39 DTI is an advanced form of MRI that is sensitive to axonal injury. Using DTI, axonal abnormalities have been found in US military personnel with blast-related mild TBI (mTBI). Substantial numbers of abnormalities were found in regions of the brain not known to be commonly injured in civilian cases of mTBI but predicted to be vulnerable to blast on the basis of computational simulations. Our goal is using these types of technologies to understand the biomolecules’ molecular pathways and mechanisms to fully understand the individuals’ injury and to decide on the proper course of treatment. Also, because DTI and, one day soon, liquid biopsies will be performed relatively quickly using MRI scanners positioned at sports stadiums and US military facilities and civilian hospitals, these assessments may be useful in diagnosis, triage, and treatment.
It is also vitally important to be aware of the potential for unforeseen impact as the efficacy of TBI assessment improves. While the benefits of injury treatment, and especially prevention, are self-evident, there are potential pitfalls with implementation of protocols designed to minimize risk. With the increased awareness of the dangers of concussion in the pediatric population, enrollment in youth football and other contact sports is declining precipitously.40–42 Armed services personnel experience a wide array of injuries while performing tasks essential to their duties.32 Links between TBI and PTSD are suspected and perhaps even probable. Yet, the mechanistic underpinnings of how exactly the dysregulation caused by concussive events leads to the behaviors observed in post-traumatic stress have yet to be elucidated. Discovery of a panel of definitive trauma-specific biomarkers could, and would, lead to a fuller understanding of etiology and progression. However, great care must be taken in how to use our burgeoning knowledge. Removal from participation in contact sports based on a likelihood of injury could be problematic. Determinations of ineligibility for enlistment in the armed services or imposed limitations in scope of service or in specific roles that result from pre-emptive testing could have profound negative effects on the culture of service and sacrifice inherent in our military. The costs in manpower and personnel have the potential to be significant. Therefore, we must tread carefully in how we use and implement the knowledge that we acquire through the advancements in our methodologies.
Acknowledgments
The authors thank Loma Linda University School of Medicine and the Center for Health Disparities and Molecular Medicine for supporting this work.
References
Footnotes
Contributors RBM: conceptualization, writing-original draft. PAV and RNF: preparation of table 1, review and editing. NRW: conceptualization, funding, project administration, resources, software, supervision, writing-original draft, review and editing.
Funding Research reported in this publication was supported by a Loma Linda University internal Grants to Promote Collaborative and Translational Research (GCAT) mechanism.
Competing interests None declared.
Patient consent for publication Not required.
Provenance and peer review Not commissioned; externally peer reviewed.