Article Text
Abstract
Resuscitative endovascular balloon occlusion of the aorta (REBOA) has become an increasingly popular alternative to emergency thoracotomy and aortic cross-clamping in patients with exsanguinating hemorrhage.1 This new capability is increasingly being used in non-trauma situations.2 3 This report demonstrates another novel use of REBOA for iatrogenic intra-abdominal hemorrhage.
An 83-year-old man with multiple medical comorbidities and a history of chronic mesenteric ischemia was admitted to our institution for an elective mesenteric revascularization. Revascularization was unsuccessful, despite attempts to cross the lesion. Postprocedure, the patient developed a right groin hematoma, and CT on postprocedure day 0 demonstrated a femoral artery pseudoaneurysm and subintimal contrast at the level of the celiac artery, representing an iatrogenic dissection.
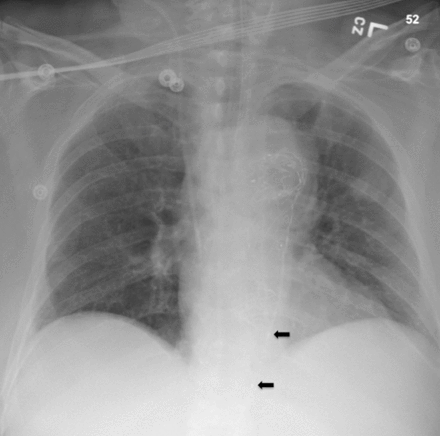
The following day, he complained of dizziness. Physical examination revealed a blood pressure of 68/35 mm Hg, heart rate of 100 beats per minute, and a distended abdomen. Because the surgical intensive care unit (SICU) was full, he was transferred to the neurotrauma intesive care unit (NTICU) and intubated for hemodynamic instability. A chest X-ray revealed a prior thoracic endovascular aortic repair (figure 1), but no intrathoracic hemorrhage or pathology. Bedside ultrasonography revealed intra-abdominal fluid. Laboratory workup showed hemoglobin of 6.1 g/dL, from 10.9 the previous day. The patient was given two units of packed red blood cells, without response. The intensive care unit (ICU) team initiated norepinephrine, with minimal improvement despite increasing doses.
Chest X-ray with catheter in zone 1. Arrows mark the proximal and distal markers of the resuscitative endovascular balloon occlusion of the aorta.
What would you do?
Transfuse two units of packed red blood cells and observe.
Proceed to the operating room (OR) for exploratory laparotomy.
Endovascular balloon occlusion of the aorta (zone 1).
- endovascular therapy
- intraabdominal hemorrhage
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
Statistics from Altmetric.com
What we did and why
After review of his prior CT angiography, it was thought that the patient was bleeding intra-abdominally secondary to a ruptured iatrogenic dissection of the celiac artery. The OR was mobilized and the general surgery team retrieved a REBOA from the emergency department. The left groin was selected for access to avoid right groin pseudoaneurysm, and the interventional radiology attending physician placed an ultrasound-guided 18-gauge left femoral artery arterial catheter, which was upsized to a 7 Fr sheath. The senior general surgery resident then inserted a REBOA (Prytime Medical, Boerne, TX) through the 7 Fr sheath to 45 cm, after flushing the catheter and testing the balloon. A chest X-ray confirmed position of the catheter within zone 1, and the balloon was inflated slowly to 8 mL with normal saline. The patient’s blood pressure subsequently improved to 180/90 mm Hg and the norepinephrine was stopped (table 1).
Time course of critical events
The patient was emergently moved to the OR for laparotomy, during which the middle colic artery was found to be bleeding, potentially due to a misplaced wire after multiple attempts to cannulate the celiac artery. The bleeding was controlled, a negative pressure wound was placed, and he was taken to the ICU. He returned to the OR 2 days later and was closed. He was ultimately discharged to a skilled nursing facility.
REBOA technology is increasingly being used in patients with traumatic injuries and its use is being actively studied. The best described indication is for traumatic injury with non-compressible torso hemorrhage.1 4 Its indications for use are broadening, including hemorrhage arising above the diaphragm and use in prehospital settings.5 6
The area of potential REBOA balloon deployment is divided into three zones. Zone 1 extends from the left subclavian artery to the celiac artery and is indicated when mesenteric bleeding was suspected, as above. Zone 2 includes the visceral vessels from the celiac artery to the most caudal renal artery. Zone 3 extends from the renal artery to the aortic bifurcation and is used in cases of pelvic or junctional/lower extremity hemorrhage.
Traumatic non-compressible torso hemorrhage is an accepted indication for zone 1 REBOA deployment. To our knowledge, REBOA has not been used in the case of iatrogenic mesenteric injury outside the OR. Immediate laparotomy or mesenteric angiography is indicated in this case, requiring a potentially dangerous transport to the OR, radiology suite or hybrid room. Application of REBOA to this clinical problem allowed for time to alert the OR and safely transport the patient.
Vascular injury is a known complication of both angiographic procedures and REBOA deployment, especially access site complications.7 Our patient had a known pseudoaneurysm, and vascular access was carefully obtained by the interventional radiology attending who was present at the patient’s bedside. Additionally, given the patient’s known atherosclerotic disease and suspected mesenteric dissection, there was a theoretical risk of additional aortic intimal damage. Additionally, in a patient with a prior aortic graft, it is important to confirm appropriate REBOA placement prior to inflation of the occlusion balloon.
Our institution is a level 1 trauma center that has used resuscitative endovascular balloon occlusion since 2011 for traumatic resuscitation and has a robust experience with REBOA. REBOA balloons are stocked in our trauma bays, in the same cart with its requisite equipment, including sterile supplies, 18-gauge arterial catheters, and 7 Fr sheaths. Our trauma faculty, fellows, and surgical residents are trained to use the technology, and our patient benefited from the experience of the surgical house staff.
The interesting aspect of this case was the utilization of REBOA in emergent truncal hemorrhage arising from an iatrogenic injury, in a hospitalized patient. Early intervention stabilized the patient and allowed time to transport the patient to the OR for definitive management.
In summary, this case demonstrates the evolving capabilities of REBOA technology and the benefits of training surgical staff and residents on its use.
Footnotes
Contributors TAC: table and figure preparation. CJG and JBH: literature review and article preparation.
Funding The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests JBH: Chief Medical Officer of Prytime Medical, Founder and Board of Directors of Decisio Health, Consultant for Terumo BCT, Medical Advisory Board of Arsenal Medical, and coinventor of the junctional emergency treatment tool.
Patient consent Obtained.
Provenance and peer review Not commissioned; externally peer reviewed.
Data sharing statement There are no relevant unpublished data.